Advertisement
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The gene editing technology CRISPR offers potential for treating both hematologic cancer and solid tumors.
“The promise with the technology is now we can use our own immune system and use it as a targeted therapy against cancer,” says Faiz Anwer, MD, a hematologist at Cleveland Clinic who leads bone marrow transplant, stem cell transplant and CAR T-cell therapy for multiple myeloma indication.
In a recent episode of Cleveland Clinic’s Cancer Advances podcast, Dr. Anwer provides an overview on the current state of CRISPR technology, including:
Advertisement
Click the podcast player above to listen to the episode now, or read on for a short edited excerpt. Check out more Cancer Advances episodes at clevelandclinic.org/podcasts/cancer-advances or wherever you get your podcasts.
Excerpt from the podcast:
Podcast host Dale Shepard, MD, PhD: When we think about this technology, give us a little bit of a background on how it’s been utilized for treating cancer so far.
Anwer: So, this is very timely because we just initiated a phase 1 clinical trial with a pharmaceutical company. It’s a multi-institute study where we’re using a cancer-fighting T cell – and T cells are immune cells. Their main job is to fight against infections as well as cancers. And through this CRISPR technology, the allogeneic cells which came from a healthy donor were modified. Those T cells are now able to find and attack and kill cancer cells. And we are using it for the treatment of multiple myeloma.
In this particular case, this cell is modified in four different ways where they have removed a T-cell receptor and inserted a new receptor, which can find a cancer target called the BCMA protein. And on the other end, through this technology, they have modified the cell, so it does not attack the patient’s body – so it does not cause graft-versus-host disease.
And they have also modified the cell in a way that the patient’s host immune system does not attack and kill the donor cell. So, it is protected from the rejection of these cells. Through these edits, now these cells can stay in the body and potentially be very effective in eradicating cancer from the body.
Advertisement

First-of-its-kind research investigates the viability of standard screening to reduce the burden of late-stage cancer diagnoses
Study demonstrates ability to reduce patients’ reliance on phlebotomies to stabilize hematocrit levels

Findings highlight an association between obesity and an increased incidence of moderate-severe disease
Cleveland Clinic Cancer Institute takes multi-faceted approach to increasing clinical trial access
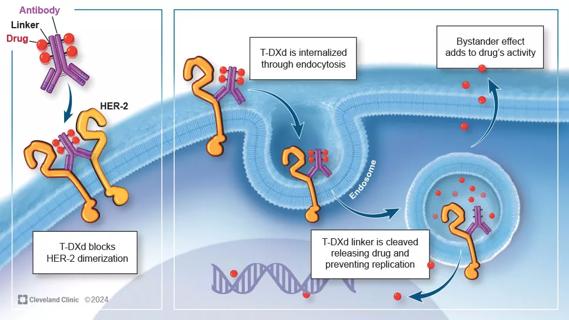
Key learnings from DESTINY trials

Study of 401,576 patients reveals differences in cancer burdens as well as overall survival

Enfortumab plus pembrolizumab reduced risk of death by 53% compared with platinum-based chemotherapy

Large cohort study finds no reduction in survival for patients managed with active surveillance compared to treated patients